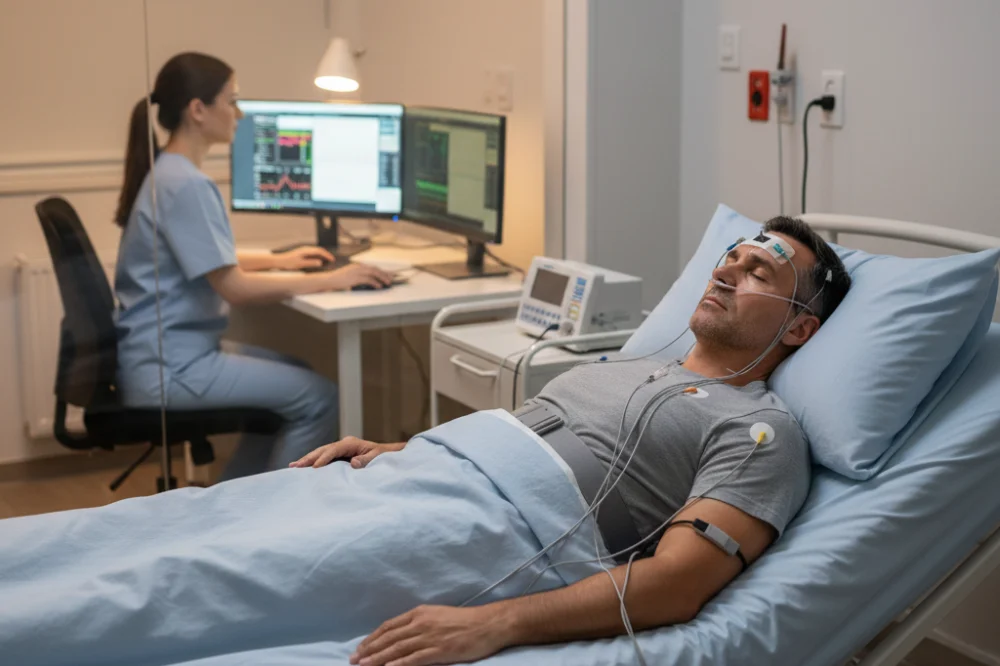
If you have been scheduled for an overnight sleep study, it is normal to feel anxious about what will happen once you arrive. Many Houston patients worry about sleeping in an unfamiliar place, being connected to wires, or not sleeping well enough for the test to work. Understanding what actually happens during an in‑lab sleep study can reduce fear and help you feel more prepared.
An in‑lab sleep study, also called polysomnography, is a painless overnight test performed in a specialized sleep center or hospital setting. It is designed to give doctors a detailed picture of how your body functions while you sleep. This article provides a clear, step‑by‑step walkthrough of the experience, from preparation to results, so you know exactly what to expect.
What Is an In‑Lab Sleep Study and Why Is It Ordered?
An in‑lab sleep study is an overnight medical test that monitors your brain activity and body systems while you sleep. Sensors track brain waves, eye movements, breathing patterns, oxygen levels, heart rhythm, limb movements, snoring, and body position. This detailed information helps doctors diagnose sleep disorders accurately.
Doctors often recommend an in‑lab study when symptoms are complex or when a home sleep test may not provide enough information. In‑lab testing is commonly used to evaluate obstructive sleep apnea, central sleep apnea, movement disorders, parasomnias, and narcolepsy. It is also used when patients have other medical conditions that require closer monitoring overnight.
Getting Ready for Your Night in the Sleep Lab
Preparing for an in‑lab sleep study is usually simple and focuses on helping you sleep as normally as possible. Patients are often asked to avoid caffeine or alcohol later in the day and to keep hair clean and free of heavy products. You can typically take your regular medications unless your provider gives different instructions.
You should bring comfortable sleepwear, toiletries, and any items that help you relax before bed, such as a book or phone charger. Many Houston sleep centers allow patients to bring their own pillow if it makes them more comfortable. Planning ahead can make the evening feel less stressful and more familiar.
Arrival and Sensor Setup
When you arrive at the sleep center, you will check in and be shown to a private room that often resembles a small hotel room. A technologist will explain the process, answer questions, and give you time to change into sleepwear. The goal is to help you feel at ease before the study begins.
The technologist then attaches sensors using gentle adhesive or paste. These sensors do not hurt, although they may feel unusual at first. Wires are long enough to allow you to turn in bed, and staff can disconnect and reconnect sensors if you need to get up during the night.
What Happens While You Sleep
Once the sensors are in place, the technologist performs a brief calibration to confirm that all signals are recording correctly. After this check, the lights are turned off and you are encouraged to sleep as normally as possible. Throughout the night, a trained technologist monitors your signals from a nearby control room to ensure safety and data quality.
- Real-time monitoring of brain activity, breathing, oxygen levels, heart rhythm, and movement
- Ongoing observation by a technologist who can respond if sensors shift or signals change
- Ability to communicate with staff through an intercom if you need help
- Assistance with bathroom breaks, including temporary disconnection and reconnection of sensors
Many patients worry that not sleeping deeply or for long enough will make the test invalid. In reality, most people sleep enough to collect accurate and useful data, even if sleep feels lighter than usual. The technologist’s role is to work with whatever sleep occurs and make adjustments as needed so the study can still provide meaningful results.
Many patients worry about not sleeping well enough for the test to be useful. In reality, most people sleep enough to collect accurate data, even if sleep feels lighter or shorter than usual. If you need to use the bathroom, staff can assist and reconnect sensors afterward.
CPAP Titration and Split‑Night Studies
Some patients may have a split‑night sleep study or CPAP titration during their visit. In a split‑night study, the first part of the night records baseline sleep and breathing. If significant sleep apnea is detected, a CPAP mask may be introduced during the second half of the night.
CPAP titration studies focus on adjusting air pressure levels to see what best controls breathing events. Technologists monitor comfort and breathing throughout the night and make changes as needed. Patients are awake when masks are fitted, and support is available if discomfort occurs.
Morning After and Getting Your Results
In the morning, patients are usually awakened early and sensors are gently removed. Most people are able to leave within an hour and resume normal daily activities. The overnight technologist collects data but does not provide a diagnosis at that time.
Your sleep study is later reviewed and interpreted by a sleep physician. Results are typically discussed during a follow‑up visit or call, where findings and treatment options are explained clearly. This step ensures you understand both the diagnosis and the recommended next steps.
Who May Be Asked to Have an In‑Lab Sleep Study
In‑lab sleep studies are often recommended for patients whose symptoms or medical history suggest more complex sleep problems. These studies allow for close monitoring and detailed data collection throughout the night. For some people, this level of evaluation is necessary to ensure safety and accuracy.
- Patients with suspected central sleep apnea or complex breathing patterns
- Individuals with heart disease, lung disease, or neuromuscular conditions
- Children and adolescents with suspected sleep disorders
- Patients with multiple unexplained sleep complaints, such as insomnia and excessive daytime sleepiness
For patients in these situations, an in‑lab study provides information that home testing cannot. Full monitoring helps doctors make accurate diagnoses and avoid missed conditions. When there is uncertainty, in‑lab testing is often the safest option.
In‑Lab Sleep Studies in Houston, TX
Houston sleep centers offer a range of in‑lab studies, including full polysomnography, split‑night studies, CPAP titration, and daytime testing when needed. Many centers are equipped to handle medically complex patients and provide overnight technologist supervision. These studies are considered the gold standard for diagnosing complex or unclear sleep disorders.
Local centers often help patients with scheduling, insurance authorization, and follow‑up planning. Some Houston facilities also coordinate results with dentists and other providers involved in airway or sleep‑related care. This team‑based approach helps connect diagnosis with effective treatment.
In‑Lab vs Home Sleep Testing at a Glance
Both in‑lab and home sleep tests play important roles in diagnosing sleep apnea. The right choice depends on symptoms, medical history, and the level of detail needed. Understanding the difference can help patients feel confident about why a specific test was recommended.
| Feature | In‑Lab Sleep Study | Home Sleep Apnea Test |
| Setting | Sleep center or hospital | Patient’s home |
| Data collected | Full brain and body monitoring | Breathing and oxygen data |
| Best for | Complex or unclear cases | Uncomplicated adults |
| Supervision | Continuous technologist monitoring | Limited, device‑based |
In‑lab studies provide the most detailed information and are often used when safety or complexity is a concern. Home tests offer convenience for select patients but are not a replacement in every situation. Your provider’s recommendation is based on choosing the safest and most accurate option for you.
What Happens After Diagnosis
A diagnosis is the beginning of care, not the end. Once results are reviewed, your provider will discuss treatment options based on the type and severity of your sleep disorder. These options may include CPAP therapy, oral appliance therapy, lifestyle changes, or referral to other specialists.
Follow‑up care is essential to ensure treatment is effective. Adjustments may be needed, and repeat testing is sometimes used to confirm improvement. Coordinated care between sleep physicians and other providers supports long‑term health and better sleep.
Frequently Asked Questions
Does an in-lab sleep study hurt?
No, an in-lab sleep study is painless and non-invasive. Sensors are attached to the skin using adhesive or paste and do not involve needles or any procedures that cause pain. Most discomfort people notice comes from sleeping in a new environment rather than from the equipment itself.
What if I cannot fall asleep during the study?
It is very common to sleep less than usual during an overnight sleep study. Even partial or lighter sleep is often enough for doctors to collect accurate and useful data. Sleep technologists are trained to work with whatever sleep you are able to get and can still obtain meaningful results.
Can I get up to use the bathroom during the night?
Yes, you can get up to use the bathroom if needed. A technologist can temporarily disconnect the sensors and help reconnect them afterward. Your comfort, safety, and dignity are always a priority throughout the study.
How long does it take to get sleep study results?
Results are not provided immediately the next morning. A sleep physician reviews and interprets the data after the study, which usually takes several days. Your provider will then review the results with you and explain the findings and recommended next steps.